There are numerous reports about the epidemiology and treatment patterns of people with serious mental illness, but comparatively few about people with mild to moderate mental illness (MMMI). Enter Valerie Hoffman, our VP of Intervention Science, who just presented a poster at the American Society of Clinical Psychopharmacology (ASCP) Conference detailing nationally representative estimates and correlates of MMMI among U.S. adults. In this latest Chats with Woeboteers, Valerie reveals the study’s key findings, and how they can help guide the industry’s understanding about optimizing support and treatment equity and capacity.
Why did you want to take a deeper look at people with MMMI?
Overall we wanted to better understand potential disparities and underserved populations. So the study focused on the prevalence, mental health support and services landscapes, and the unmet need and barriers to care among U.S. adults with mild to moderate levels of mental illness, or MMMI. We also looked at the correlates of MMMI in terms of who was more or less likely to get support and services and to have an unmet need for care.
Is the focus on uncovering the unmet need in MMMI new?
The study, which we’re expecting will be published in the peer reviewed literature, is the first known comprehensive look at the MMMI landscape: who has it, who’s getting services and what type are they getting, who has a perceived unmet need for care, and what are the barriers to care that are precluding them from getting the right support. Most studies lump all of those who have any mental illness together, so separating out MMMI from serious mental illness gives us a much better understanding of care needs. It’s a huge area. We found that MMMI affects more than three times as many adults as serious mental illness. So the burden is quite substantial, and warranted a deeper look.
Why this study, now?
We know that rates of mental illness continue to rise, even post pandemic. But we need to know more about people with MMMI to get a sense of the overall burden and to identify the specific characteristics of people and what might help them.
How did you do the analysis?
We analyzed data from adults aged 18 and older who participated in the 2021 National Survey on Drug Use and Health, a representative survey conducted annually that estimates the number of adults with any mental illness in the past year based on mental disorders from the DSM. Our analysis focused on those who specifically met the criteria for MMMI, which differed from serious mental illness based on the level of functional impairment.
What did you find?
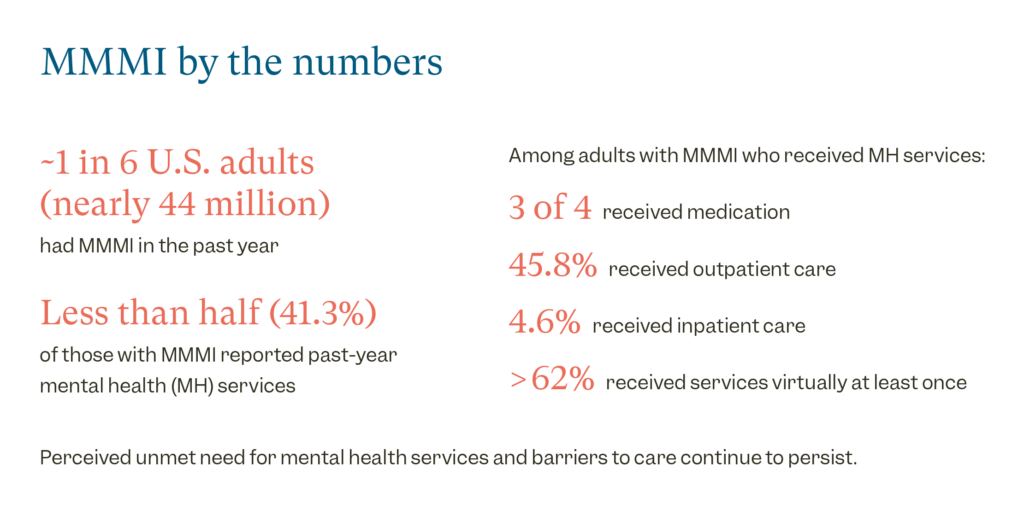
The scale of the issue in terms of the unmet need is staggering. Almost 44 million adults in the U.S., or one in six, are estimated to have had MMMI in the past year. And among those, less than half, just over 41%, reported any sort of mental health service. That means more than half of those living with MMMI are not getting care. Among those who did receive a service we saw that three quarters of them received medication, nearly half received some sort of outpatient care and just 5% reported some type of inpatient mental health care. Interestingly, we found 62% of those who did receive a service got some sort of virtual care.
What did you find about the actual people who are, or aren’t, getting care?
Those less likely to receive care included males, not Hispanic/Latino Black/African American, not Hispanic/Latino Asian, and Hispanic/Latino adults versus not Hispanic/Latino White adults. Those less likely to receive care were also uninsured and had a high school education or less. Nearly one in five of those with MMMI who didn’t receive care reported perceiving needing it. And nearly all of those who reported at least one barrier to receiving care said that cost, not knowing where to go for services, and not having time to get services were the biggest barriers.
That’s dismaying, to say the least.
It is. But this is the first really clear view that people with MMMI—especially in vulnerable populations—still have very real needs for mental health care that aren’t being addressed. As a nation we can, and must, do better. One interesting point is that the rate of those receiving virtual care is so high. These data were from 2021, but I’ve taken a peek at the 2022 data and it’s appears to be even higher. So it seems that the trend toward virtual delivery of mental health support is here to stay. Hopefully that can help address some of the most commonly cited barriers to care.
Where do we go from here?
We’ll be taking a deeper look to match the characteristics of those who would best benefit from using an appropriate support tool to maximize their mental health. Despite the increased use of virtual services, our findings suggest there is more to do to improve access to low-cost, easily accessible, on-demand mental health support tools to optimize well-being. The ultimate aim would be to study the most underserved populations so we can help bring those types of services to the people with the greatest need.